Mental Health, Mitochondria, & Nutrition: An Understated Correlation
When one thinks about mental health, the idea of energy production at the cellular level is not the first consideration. According to Dr. Sundeep Dugar, pharmaceutical chemist and co-founder of BlueOakNx, and Robert Lustig, MD, MSL, Professor Emeritus of Pediatrics, Endocrinology at UCSF, that might be exactly where one might need to look.
This conversation was inspired at the 2025 Integrated Medicine for Mental Health Conference in San Diego, when Dr. Dugar talked about a systems approach to understanding the centrality of the role of mitochondria in mental health when combined with the correct nutrition.
The Brain's Massive Energy Demands
Here is a matter of fact: the brain represents only about two percent of total body mass, yet it consumes twenty one percent of energy to maintain the body. Even more surprising? The brain actually uses more energy when sleeping than when awake. This energy demand is met by the mitochondria which both fuel and protect the energy production of the cell.
Each neuron in the brain contains an estimated 2 million mitochondria. Two million energy-producing factories working around the clock in every single brain cell to power everything from memory storage to emotional regulation.
The following slide demonstrates the distribution of energy and how mass is not the determinant to the expenditure of energy.
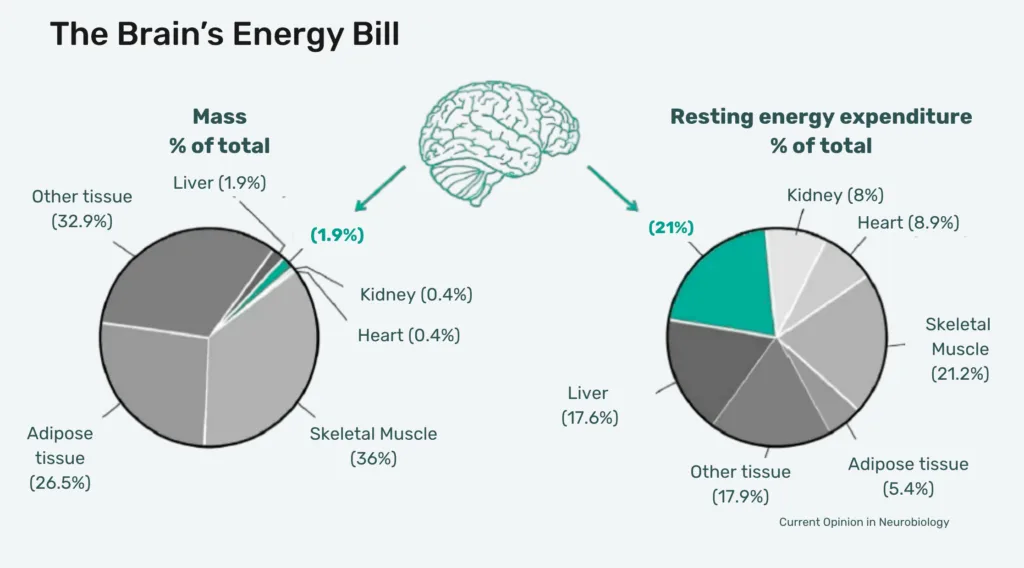
Dr. Dugar also talked about the process of aging, which is driven by the mitochondria. The body reaches peak mitochondrial capacity at age 21; From there on, humans lose 10 to 15% of mitochondrial capacity every decade. Dr. Dugar explains. “That’s when you start losing muscle strength. The metabolism slows down. No matter how hard you try, you gain weight. As you get older, you start losing memory.”
The Mitochondria Mental Health Connection
Mitochondria produce approximately 95% of the Adenosine Triphosphate (ATP) the body needs for all biological processes. When mitochondrial function and quantity declines, so does the brain’s ability to function optimally.
Dysfunctional mitochondria create a cascade of problems, including:
- Producing an excess Reactive Oxygen Species (ROS)
- Activating inflammatory pathways through NF-kappa Bs
- Inducing neuroinflammation and oxidative stress, which in turn manifests as mental health challenges.
Connection of Nutrition to Mitochondria Quality and Function
Dr. Robert Lustig, pediatric endocrinologist and author of the book titled, Metabolic, joins the discussion to explain how modern diets are literally poisoning the mitochondria. Ultra-processed foods and especially fructose, the sweet component of sugar, are particularly toxic to mitochondrial function.
The image here is an example of a balanced and nutritious diet for the mitochondria.

He explains that the body doesn’t metabolize fructose the way it does glucose. Instead, excess fructose gets stored, and this accumulation plays a significant role in various pathologies.
Research has shown dramatic results when fructose is removed from the diet. In one study at UCSF, children with metabolic syndrome who clearly had mitochondrial dysfunction showed significantly elevated lactate levels. When researchers removed fructose from their diet and replaced it with starch (keeping calories equal), their lactate levels dropped by 50%. This simple dietary change improved their mitochondrial function measurably.
Understanding and supporting mitochondrial function through a healthy diet and a systemic health regime adding movement, may be the key to addressing the mental health crisis from its energetic roots.
Watch Dr. Dugar’s presentation to learn more about a sterioisomer that could provide cellular signals to, and help rebuild mitochondrial capacity. As mitochondrial function improves, baseline cellular energy increases, potentially reducing mental health disparity and creating a positive upward cycle instead of the current negative spiral.
Read / Watch More
- Read more about Mitochondria, Metabolism and Mental Health
- Learn more about the role of mitochondrial dysfunction in Autism Spectrum Disorders
- Save the Date for an educational Symposium presented by the New York Academy of Sciences and BlueOakNx on Mitochondrial Health & Healthspan: Brain Metabolism and Bioenergetics.

